Nanotechnology in Medicine: Targeted Drug Delivery
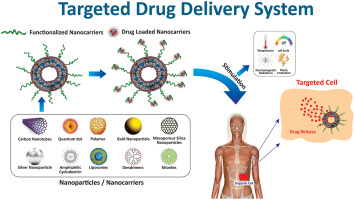
Nanotechnology, the manipulation of matter at the atomic and molecular scale, is revolutionizing medicine, particularly in the realm of targeted drug delivery. This technology offers unprecedented precision in treating diseases, promising to enhance the efficacy of treatments while minimizing side effects. This blog delves into the principles of nanotechnology in medicine, the mechanisms and benefits of targeted drug delivery, current applications, and the challenges that must be overcome for widespread adoption.
Understanding Nanotechnology in Medicine
Nanotechnology involves creating and utilizing structures, devices, and systems by controlling shape and size at the nanometer scale (1-100 nanometers). In medicine, nanotechnology enables the development of nanoparticles that can interact with biological molecules at the cellular and molecular level, allowing for precise intervention in disease processes.
Key Benefits of Targeted Drug Delivery
- Increased Efficacy Nanoparticles can be engineered to deliver drugs directly to diseased cells or tissues, enhancing the concentration of the therapeutic agent at the target site. This increases the drug’s efficacy and allows for lower doses, reducing the risk of side effects.
- Reduced Side Effects Traditional drug delivery methods often affect healthy tissues along with diseased ones, causing adverse side effects. Targeted delivery minimizes exposure to healthy cells, thus significantly reducing the occurrence of side effects and improving patient quality of life.
- Improved Pharmacokinetics Nanoparticles can be designed to improve the pharmacokinetic properties of drugs, such as solubility, stability, and half-life. This allows for better absorption, distribution, metabolism, and excretion of the therapeutic agents, optimizing their therapeutic potential.
- Controlled Release Nanoparticles can be engineered to release drugs in a controlled manner, maintaining therapeutic levels over extended periods. This is particularly beneficial for chronic diseases requiring sustained drug release, reducing the frequency of administration and improving patient compliance.
- Enhanced Targeting Capabilities Advanced targeting mechanisms, such as surface modifications with ligands or antibodies, enable nanoparticles to home in on specific cell types or receptors. This specificity enhances the therapeutic index of drugs and opens new avenues for personalized medicine.
Mechanisms of Targeted Drug Delivery
- Passive Targeting Passive targeting leverages the enhanced permeability and retention (EPR) effect, where nanoparticles accumulate in tumor tissues due to their leaky vasculature and poor lymphatic drainage. This allows nanoparticles to preferentially localize in tumor sites, delivering higher drug concentrations to cancer cells.
- Active Targeting Active targeting involves modifying the surface of nanoparticles with molecules such as antibodies, peptides, or small molecules that bind specifically to receptors on the target cells. This ensures that the nanoparticles are directed precisely to the diseased cells, enhancing treatment specificity.
- Stimuli-Responsive Delivery Nanoparticles can be designed to respond to specific stimuli in the body, such as pH, temperature, or enzymes, triggering the release of the drug at the desired site. For example, nanoparticles can release their payload in the acidic environment of a tumor, ensuring that the drug is released precisely where it is needed.
Current Applications of Nanotechnology in Targeted Drug Delivery
- Cancer Treatment Cancer treatment is one of the most prominent areas where nanotechnology has made significant strides. Nanoparticles loaded with chemotherapeutic agents can selectively target cancer cells, minimizing damage to healthy tissues. For instance, liposomal doxorubicin (Doxil) is a nanoparticle formulation used to treat ovarian cancer and Kaposi’s sarcoma, offering improved safety and efficacy over conventional doxorubicin.
- Cardiovascular Diseases Nanoparticles are being developed to target atherosclerotic plaques, delivering drugs that can stabilize or reduce these plaques and prevent heart attacks. Additionally, nanoparticles can be used to deliver therapeutic agents to repair damaged heart tissue following myocardial infarction.
- Neurological Disorders Overcoming the blood-brain barrier is a significant challenge in treating neurological disorders. Nanoparticles can be engineered to cross this barrier and deliver drugs directly to the brain, offering new treatment options for diseases such as Alzheimer’s, Parkinson’s, and brain tumors.
- Infectious Diseases Nanoparticles can enhance the delivery of antibiotics and antiviral drugs, improving their efficacy against resistant strains and reducing toxicity. For example, nanoparticle formulations of antiretroviral drugs are being explored for the treatment of HIV, aiming to improve drug delivery to infected cells and reduce viral load.
- Gene Therapy Nanotechnology is also advancing gene therapy by enabling the delivery of genetic material to specific cells. Nanoparticles can protect DNA or RNA from degradation and facilitate its entry into target cells, offering potential cures for genetic disorders.
Challenges and Future Directions
- Safety and Toxicity The safety and potential toxicity of nanoparticles are major concerns. Long-term studies are needed to assess the biocompatibility and potential side effects of nanoparticles, including their accumulation in tissues and organs.
- Scalability and Manufacturing Producing nanoparticles with consistent quality and in sufficient quantities for clinical use is challenging. Developing scalable and cost-effective manufacturing processes is essential for the widespread adoption of nanotechnology in medicine.
- Regulatory Approval The regulatory pathways for nanoparticle-based therapies are complex, requiring rigorous testing to ensure safety and efficacy. Clear guidelines and standards are needed to streamline the approval process and facilitate the translation of nanotechnology from the lab to the clinic.
- Targeting Precision Enhancing the precision of targeted drug delivery remains a key challenge. Research is ongoing to improve the specificity and efficiency of nanoparticles, including the development of multifunctional nanoparticles that can target multiple disease markers simultaneously.
- Public Acceptance and Ethical Considerations Public perception and ethical considerations play a significant role in the adoption of new medical technologies. Transparent communication about the benefits and risks of nanotechnology, along with addressing ethical concerns, is crucial for gaining public trust and acceptance.
Nanotechnology is poised to revolutionize medicine through targeted drug delivery, offering new hope for treating a wide range of diseases with unprecedented precision and efficacy. While significant challenges remain, ongoing research and innovation are paving the way for safer, more effective, and personalized treatments. As the field continues to evolve, the promise of nanotechnology in medicine holds the potential to transform healthcare and improve patient outcomes across the globe.
Stay ahead with ITBusinessNews – Your trusted source for Technology and Business news. Fast & Precise





